What is Bladder Cancer?
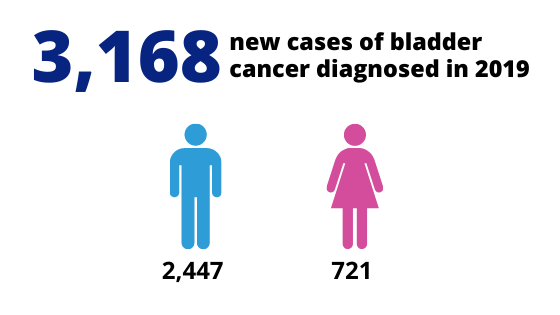
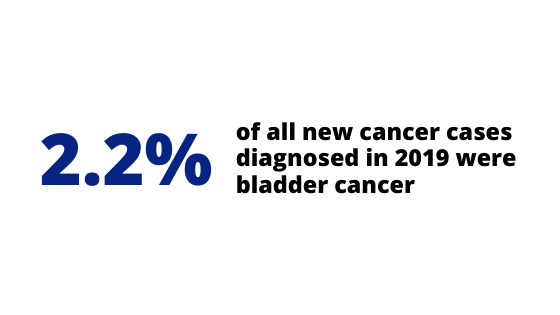
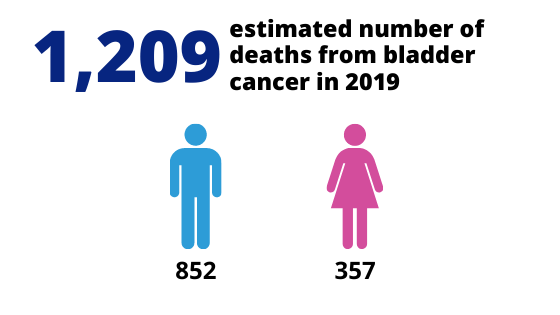
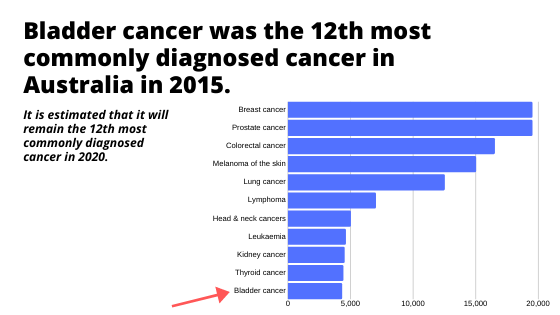
Did you know that about 1 in every 110 men will be diagnosed with bladder cancer before age 75? Bladder cancer is one of the most common cancers in men. In Australia, almost 3100 people are diagnosed with bladder cancer every year. As such, awareness and education on this topic is important.
Bladder cancer starts when cells in the inner lining of the bladder, called the urothelium, begin to grow abnormally and multiply uncontrollably. As the cancer advances, it can spread deeper into the layers of the bladder wall. Additionally, some cancer cells may break away and travel to other parts of the body, a process known as metastasis.
If you or a loved one is suspected or has been diagnosed with bladder cancer, we understand that this could be a challenging and emotional time for you. Don’t worry; we’re here to offer guidance and enlightenment. It’s best to arm yourself with knowledge and expert medical advice during this time. We highly encourage you to seek professional help from urologists such as Dr. Katelaris to help you better understand this condition. Remember: awareness and timely medical intervention are critical in navigating and overcoming bladder cancer.
Types of Bladder Cancer
There are three main types of bladder cancer, each named after the type of cell where the cancer begins:
- Urothelial Carcinoma (80–90% of all bladder cancers) – This type starts in the urothelial cells that line the bladder wall. It’s also known as transitional cell carcinoma.
- Squamous Cell Carcinoma (1–2% of all bladder cancers) – Begins in the thin, flat squamous cells that make up part of the bladder lining. This form of cancer is often more invasive.
- Adenocarcinoma (About 1% of all bladder cancers) – Forms in the glandular cells of the bladder and is typically invasive.
Each type of bladder cancer has unique characteristics and requires specific treatment approaches. If you are diagnosed with bladder cancer, your urologist will explore various treatment options.
Dr. Katelaris is an expert urological surgeon who deals with bladder cancer treatment in Sydney. Using the most current surgical techniques and technologies, Dr. Katelaris provides personalised treatment plans tailored to the unique needs of each patient.
On this information page, you can learn about the following:
- Signs and Symptoms of Bladder Cancer
- Factors Affecting Bladder Cancer Prognosis and Treatment Options
- Bladder Cancer Diagnosis & Screening
- Stages of Bladder Cancer
- Bladder Cancer Treatment Options Per Stage
- Research and Clinical Trials
- Risks & Prevention
- Patient Stories
- FAQs
Next, we will discuss the signs and symptoms of bladder cancer, which are crucial for early detection and treatment.
Signs and Symptoms of Bladder Cancer
Bladder cancer can be difficult to detect in its early stages. That’s why recognising the signs and symptoms early on can lead to more timely detection and improved treatment outcomes.
Have you noticed blood in your urine? The most common symptom of bladder cancer is hematuria or blood in the urine, which can be visible to the naked eye or detectable only under a microscope. While hematuria can indicate less serious issues like urinary tract infections or kidney stones, it’s important to have it checked by a healthcare professional.
Other notable symptoms include:
- Increased frequency of urination without an increase in volume.
- Urgent need to urinate.
- Pain or burning during urination.
- Difficulty urinating or having a weak urine stream.
Advanced Bladder Cancer Symptoms
What happens when bladder cancer advances? As the cancer progresses, more severe symptoms may develop, especially if the disease spreads beyond the bladder. These can include:
- Pelvic or back pain
- Inability to urinate
- Swelling in the lower extremities
- Loss of appetite and weight loss
- General feeling of weakness and fatigue
Understanding and recognising these bladder cancer symptoms is essential for getting an early diagnosis and starting the right treatment.
Some men begin noticing blood in their urine and dismiss it as a minor issue. Eventually, they get diagnosed with bladder cancer. Early detection and treatment will allow you to combat this disease successfully.
If you or someone you know shows any of these symptoms, seeing a bladder cancer specialist for a detailed check-up and tests is important. Early detection is key for successful treatment and greatly improves your bladder cancer prognosis.
Dr. Katelaris is a bladder cancer specialist in Sydney. He has extensive experience diagnosing and treating this type of cancer and offers a full range of treatment options suited to your case and condition.
Several factors can affect the prognosis and treatment options for bladder cancer. Let’s explore these factors next.
Factors Affecting Bladder Cancer Prognosis and Treatment Options
Prognosis refers to the likely outcome of a disease. While you might want to talk about your prognosis with your doctor, it’s important to understand that predicting the exact progression of the disease is impossible.
Your prognosis, chance of recovery, and treatment options for bladder cancer depend on several factors, such as:
Stage and Grade of the Cancer
What exactly does the cancer stage tell us? It shows how much the cancer has grown and whether it has spread. And how about the grade of the tumor? The grade of the tumor indicates how much the cancer cells differ from normal cells and how quickly they are likely to grow and spread.
Patient’s Overall Health and Comorbidities
Older patients or those with significant other health issues may not be candidates for aggressive surgical options or might experience more complications from certain treatments.
Treatment Response
How well the cancer reacts to the first treatments can affect both the disease outcome for the patient and the next steps in bladder cancer treatment.
Understanding these factors can help patients and healthcare providers make informed decisions about the suitable bladder cancer treatment option for you. Generally, the sooner bladder cancer is detected, the better your chances will be.
But how is bladder cancer detected? Let’s discuss the diagnostic and screening process, which is crucial for early detection.
Bladder Cancer Diagnosis & Screening
Early bladder cancer diagnosis not only broadens the treatment options available but also significantly enhances the likelihood of successful treatment outcomes.
If your doctor suspects you might have bladder cancer, they will check you and set up some tests. These tests include:
- General tests to see how your body is working overall.
- Advanced tests to find any signs of cancer.
- More tests to check if the cancer has spread.
General Tests
Physical Examination for Bladder Cancer
Since the bladder is close to the rectum and vagina, your doctor might check these areas. They do this by gently inserting a gloved finger into the rectum or vagina to feel for anything unusual. This test might feel a bit awkward or uncomfortable, but it only lasts a few seconds. Sometimes, you might not need this test until after they confirm you have bladder cancer.
Blood and Urine Tests
Your doctor will also take some blood to see how your overall health is. You’ll need to give a urine sample too. They’ll check this urine for blood and bacteria. If they find blood in your urine, you might have to give urine samples for three days continuously. These will be further checked for cancer cells.
Standard Tests
The main test to check for bladder cancer is through cystoscopy, a medical procedure examining the inside of the bladder and urethra. Before this test, you might have an ultrasound. During the cystoscopy, the doctor might also take a small tissue sample (biopsy) from your bladder. You might also need a CT or MRI scan.
Here are other tests for accurate bladder cancer diagnosis:
- Ultrasound
- Flexible cystoscopy
- Rigid cystoscopy and biopsy
- CT scan
- MRI scan
- Radioisotope bone scan
- X-rays
- PET–CT scan
Early detection is key, and bladder cancer diagnosis often involves a combination of urine tests, imaging, and biopsy.
Accurate diagnosis is essential for effective treatment planning. Once the diagnosis is in, bladder cancer staging takes place. Bladder cancer staging describes how much cancer has spread within the bladder or to other parts of the body.
Stages of Bladder Cancer
One would ask, what are the different stages of cancer, and how do they differ in severity? Let’s find out.
Understanding the stages of bladder cancer helps determine the most effective treatment plan and predict patient outcomes.
Here’s an overview of each stage:
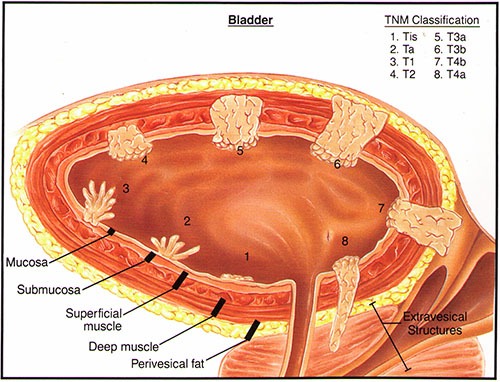
Stage 0: Cancer cells are found only on the surface of the inner lining of the bladder.

Stage 0 bladder cancer, also known as noninvasive bladder cancer, is the earliest form of bladder cancer. At this stage, the cancer cells are only found in the tissue that lines the inside of the bladder and has not spread deeper into the bladder walls.
Stage I: Cancer has begun to grow into the deeper layers of the bladder wall but has not reached the muscle layer.

Stage I bladder cancer is also called non-muscle-invasive bladder cancer. At this stage, the cancer is growing but still contained within the layers close to the inside surface of the bladder, without involving the deeper, muscular part of the bladder wall.
Stage II: Cancer has spread to the muscle layer of the bladder.

Stage II bladder cancer, also known as muscle-invasive bladder cancer, means that the cancer cells have grown deeper into the walls of the bladder, involving the muscles that help the bladder contract and release urine.
Stage III: Cancer has extended through the bladder to the fatty layer and may have spread to nearby reproductive organs (prostate, uterus, vagina).

Stage IIIA bladder cancer marks considerable growth of the disease. There could be two scenarios. 1) the cancer extends through the bladder wall into surrounding fat and possibly affects reproductive organs without reaching the lymph nodes. Or 2) the cancer spreads to a single lymph node in the pelvis but stays away from major blood vessels.

Stage IIIB bladder cancer shows a more serious progression with significant spread to the lymph nodes. There could be two scenarios: 1) the cancer reaches multiple lymph nodes in the pelvis, away from the major common iliac arteries. Or 2) the cancer involves at least one lymph node close to these key blood vessels, indicating a critical expansion near vital structures.
Stage IV: Cancer has spread to the wall of the abdomen or pelvis, distant lymph nodes, or other parts of the body.

Stage IV bladder cancer is categorised into stages IVA and IVB, marking advanced cancer progression. In stage IVA, the cancer has either spread to the abdominal or pelvic wall or reached lymph nodes above the pelvis’s common iliac arteries. In Stage IVB, the cancer has metastasised to distant organs like the lungs, bones, or liver. This type of cancer, known as metastatic bladder cancer, occurs when cancer cells travel through the lymphatic system or bloodstream to form new tumors. These tumors are made of bladder cancer cells, even if they are located in other organs like the lungs.
Each stage of bladder cancer can vary significantly in terms of treatment options and outcomes. Early stages often have a higher rate of successful treatment and a better prognosis, highlighting the importance of early bladder cancer detection and diagnosis.
Whether you are in the early stages of bladder cancer or facing more advanced challenges, Dr. Katelaris can guide you through your treatment options, ensuring you receive the highest standard of care. He has extensive knowledge and experience in different kinds of bladder cancer treatment in Sydney. His commitment to patient education and support throughout the treatment process makes him a trusted partner in managing your health.
Bladder Cancer Treatment Options
Once the stage has been determined, what are your treatment options? The stage of your cancer will affect the most appropriate treatment plan for you. Let’s discuss what your options are.
Bladder cancer treatment depends heavily on the stage at diagnosis but typically includes one or more of the following:
| Treatment | Stage | Description |
| Surgery | 0, I | One of the most common treatments, especially for noninvasive cancers. Advancements in bladder cancer surgery in Sydney offer patients several minimally invasive options that can help reduce recovery times and improve outcomes. Talk to your bladder cancer surgeon about your options. |
| Intravesical therapy | 0, I | This treatment involves placing drugs directly into the bladder through a catheter. It is primarily used for early-stage cancers to prevent recurrence. |
| Radical cystectomy | I, II, III | Removes the whole bladder if there’s a high risk of cancer returning or spreading. |
| Chemotherapy | II, III, IV | Used before surgery to shrink tumors or after to kill any remaining cancer cells. It can also be combined with radiation therapy. |
| Radiation therapy | III, IV | Uses high-energy rays to kill cancer cells, often combined with chemotherapy. Also used for patients who are not good candidates for surgery. |
| Immunotherapy | IV | A newer form of treatment that helps the immune system recognise and attack cancer cells. |
| Palliative care | IV | Focuses on relieving symptoms and improving quality of life for advanced cancer patients. |
Each treatment option has its benefits and considerations, and discussing these with your healthcare provider can help determine the best plan for you.
At Katelaris Urology, we provide a comprehensive range of appropriate bladder cancer treatments for each grade and stage. Dr. Katelaris is one of the best and most experienced bladder cancer specialists in Sydney. With him, you will be carefully supported throughout the process, and each treatment option will be carefully explained and discussed.
Aside from standard treatments, clinical trials also offer access to new and innovative therapies that might not be widely available yet. Participating in these trials can be an important option to consider as well. Let’s look at the current research and clinical trials that can also be available to you.
Research and Clinical Trials in Bladder Cancer
We can all agree that improving our understanding of bladder cancer is beneficial in improving our chances of curing this condition completely. Continuous research and clinical trials are important in the fight against bladder cancer. These efforts are crucial to developing new treatments and enhancing existing ones. The goal is to increase survival rates and improve the quality of life for patients. Through these advancements, we can offer hope and better outcomes for bladder cancer patients.
So, what’s new in bladder cancer research? Here’s a brief look at the main areas of focus in bladder cancer research today:
Current Focus Areas
- Genetic research: Identifying genetic mutations and variations that increase the risk of bladder cancer can help in developing targeted therapy.
- Immunotherapy research: This area is particularly promising, as researchers are exploring different ways to enhance the immune system’s ability to fight cancer cells.
- Combination therapies: Studies are examining the effectiveness of combining various treatments, such as chemotherapy, radiation therapy, and immunotherapy, to improve outcomes.
- Noninvasive treatments: Developing bladder cancer treatments that are less invasive than current options, thereby reducing side effects and recovery times.
Clinical Trials
Clinical trials are essential for testing the safety and effectiveness of new bladder cancer treatments and interventions before they are widely available. They offer patients access to cutting-edge therapies and contribute to the medical community’s understanding of bladder cancer in several ways:
- Phase I trials test a new drug or treatment in a small group of people for the first time to evaluate its safety, determine a safe dosage range, and identify side effects.
- Phase II trials involve administering the drug to a larger group of people to determine its effectiveness and further evaluate its safety.
- Phase III trials expand this testing to even larger groups to confirm effectiveness, monitor side effects, compare it to commonly used treatments, and collect information that will allow the drug or treatment to be used safely.
Continuous research and participation in clinical trials are vital for developing new and effective bladder cancer treatments.
For those diagnosed or at risk, advancing treatment options is crucial, but prevention remains the best strategy. Understanding the risks and preventive measures can empower you and your loved ones to take proactive steps in maintaining your health.
Let’s explore what you can do to prevent bladder cancer from occurring.
MAKE AN ENQUIRY OR REQUEST A SECOND OPINION
Risks and Prevention of Bladder Cancer
Why is one more likely to get bladder cancer? Bladder cancer causes are multifaceted. Bladder cancer, like many other cancers, is influenced by a combination of genetic, environmental, and lifestyle factors. Understanding these risks can help in developing strategies for prevention or early detection. Here’s a deeper look into the risks associated with bladder cancer and preventive measures that might reduce its incidence.
Risk Factors for Bladder Cancer
Several factors can increase the risk of developing bladder cancer:
- Smoking: This is the single greatest risk factor for bladder cancer. Smokers are at least three times as likely to get bladder cancer as non-smokers.
- Occupational exposure: Certain jobs that involve exposure to carcinogenic chemicals used in the dye, rubber, leather, textiles, and paint industries can increase the risk.
- Age: The risk increases with age, with most people diagnosed with bladder cancer being in their 60s or older.
- Gender: Men are about four times more likely to develop bladder cancer than women.
- Chronic bladder inflammation: Chronic urinary infections or irritations, as seen with long-term use of a urinary catheter, can increase the risk of squamous cell bladder cancer.
- Personal or family history: Those who have had bladder cancer before or have a family history of the disease are at higher risk.
- Certain treatments: Treatment with anti-cancer drugs known as cyclophosphamide or ifosfamide can increase bladder cancer risk, as can radiation treatment to the pelvis.
Preventive Measures
While not all cases of bladder cancer can be prevented, certain lifestyle changes can significantly reduce risk:
- Quit Smoking: Quitting smoking is the most effective measure someone can take to reduce their risk of bladder cancer.
- Occupational Safety: People working with chemicals should follow safety protocols to minimise exposure.
- Adequate Fluid Intake: Drinking plenty of fluids, especially water, helps dilute urinary toxins and may reduce the risk of bladder cancer.
- Healthy Diet: Some studies suggest a diet high in fruits and vegetables might help lower bladder cancer risk.
- Regular Medical Check-ups: For those at higher risk due to any of the above factors, regular medical check-ups that include discussions about urinary health could help with early detection.
By knowing the risk factors and taking steps to prevent them, people can lower their chances of getting bladder cancer or catching it early when it’s easier to treat. Awareness and education are key components in the fight against bladder cancer, as they give individuals the knowledge they need to take good care of their health.
To truly understand the impact of bladder cancer, it’s essential to listen to the experiences of those who have lived through it. Personal stories provide not only valuable insights but also encouragement and solidarity. Let’s hear from some patients who have faced bladder cancer head-on.
Frequently Asked Questions about Bladder Cancer
Bladder Cancer Treatment in Sydney
If you’re facing a diagnosis of bladder cancer and searching for expert treatment in Sydney, look no further than Katelaris Urology.
Dr. Katelaris is a renowned bladder cancer surgeon with years of experience in advanced medical care. He specialises in bladder cancer surgery in Sydney, offering personalised treatment plans that focus on the most effective outcomes for each patient. His commitment to using the latest techniques and technologies ensures that you receive the highest standard of care.
Don’t wait to take action if you or a loved one has been diagnosed with bladder cancer. Contact Katelaris Urology today to schedule a consultation with Dr. Katelaris, one of the top urologists in Sydney.
Learn more about your bladder cancer options and how Dr. Katelaris can help you achieve the best possible health outcomes for your condition. Book a visit or contact us here.
References:
Bladder cancer stages. National Cancer Institute (NCI). (2023, February 16). https://www.cancer.gov/types/bladder/stages
Cancer Council Victoria. (2022, May 3). Bladder cancer overview. Bladder Cancer – Cancer Council Victoria. https://www.cancervic.org.au/cancer-information/types-of-cancer/bladder_cancer/bladder-cancer-overview.html#:~:text=How%20common%20is%20bladder%20cancer,most%20common%20cancers%20in%20men