Affecting 12-17% of the Australian population, Overactive Bladder Syndrome is fairly common, and become more so as people age.
Overactive bladder disorder (OAB) is a debilitating urinary condition causes embarrassment and social isolation for many. It can restrict activities and impact many aspects of life.
Many sufferers do not seek treatment because they think overactive bladder dysfunction and urinary incontinence is a normal consequence of ageing.
There are various treatment options, such as Botox injection therapy, for urinary incontinence available for both men and women, and can result in a greatly improved quality of life.

Table of Contents
What is Overactive Bladder Disorder? (OAB)
Overactive bladder disorder occurs when the bladder muscle contracts without permission. It is a problem with bladder function that results in the frequent and sudden need to urinate that may be difficult to control. The urge to urinate can also be difficult to control and lead to urinary incontinence, which can be embarrassing and limit day-to-day activities.
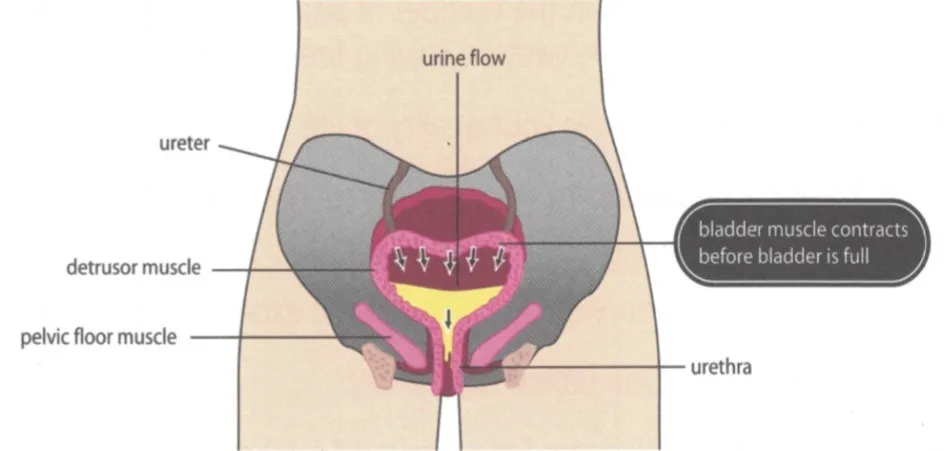
Overactive bladder disorder Overactive bladder disorder involves contraction of the bladder muscle at the wrong time resulting in urgency, frequency and urge incontinence.
Symptoms of Overactive Bladder Disorder (OAB)
- Frequency: passing urine more than 8 times per day 1
- Urgency: the sudden urge to pass urine which is difficult to ignore.
- Nocturia: waking up more than once at night to pass urine.
- Incontinence: leakage of urine that you can’t stop.
- Urge incontinence: leakage accompanied by or immediately preceded by a sudden feeling of urgency
However, men and women often present different symptoms of an Overactive Bladder.

- Men often present when nocturia becomes excessive.
- Women are more likely to experience urgency urinary incontinence or mixed urinary incontinence.
- Women tend to present when urge urinary incontinence develops and their quality of life is affected.
Causes of Overactive Bladder Disorder (OAB)
The common causes of Overactive Bladder Disorder include but are not limited to:
- Nerve damage caused by injury, disease or surgery
- Diabetes
- Urinary tract infection
- Side effects from certain types of medication
- Diuretics with caffeine
- Pregnancy
- Inflammation of the prostate
- MS or Parkinson’s disease
Diagnosis of Overactive Bladder Disorder (OAB)
For some patients, urodynamic testing is necessary to achieve the best outcome for bladder control. This is a sophisticated diagnostic procedure that enables a precise diagnosis of the causes of bladder symptoms.
This study takes half an hour and involves the passage of a small computer probe through the urethra into the bladder to measure bladder pressures and to detect bladder contractions.
Urodynamic testing and non-anaesthetic flexible cystoscopy are performed by Dr Katelaris in the urology outpatient clinic at Palmerston Road, Hornsby.
Treatment for Overactive Bladder Disorder (OAB)
If the symptoms are mild, conservation therapies or pelvic floor training can be used at treatment options.
If bladder training doesn’t work on its own, we use medication. However, if there is no response to bladder training or medication, Bladder Botox Injection can be a very effective treatment to resolve the symptoms.
The symptoms of OAB can coexist with other bladder conditions: in women, especially stress incontinence. It is important to manage both conditions. For the management of stress incontinence weight loss, pelvic floor training and minimally invasive suburethral sling surgery is available.
There are four main OAB treatments:

Conservative Therapies
Conservative therapies are an effective non-invasive urinary incontinence treatment for many women.
The many conservative therapies include:
- Bladder Retraining: Drinking 2L of water/day and progressively deferring bladder emptying for longer periods of time.
- Changing your Diet and Lifestyle: Minimising caffeinated drinks, cutting out processed foods, reducing stress.

Pelvic Floor Training
Pelvic floor training is an important part of treatment. It aids with stress leakage of urine and for women with urinary urgency, helps to suppress the bladder contraction that results in urgency and even urges incontinence.
You can learn more about Pelvic Floor Training here.

Medication
There are a number of modern medications that are proving very effective for the management of OAB. A patient can be prescribed tablets to be taken on a daily basis to decrease the urgency to urinate by lowering the bladder pressure.

Bladder Botox Therapy
Bladder Botox Therapy for OAB is generally reserved as a last resort. This is reserved for when a patience bladder condition does not respond to bladder training, pelvic floor exercises, or oral medication.
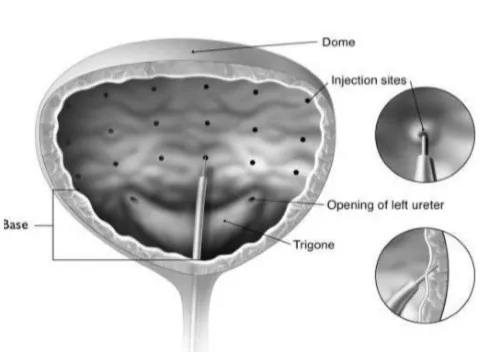
Botox is injected into multiple sites throughout the bladder and prevents the bladder muscle from aberrantly contracting.
How Does Bladder Botox Therapy Work?
Botox therapy works by reducing the ability of the bladder muscle to contract by interfering with the chemical signalling between nerves and muscles. The Botox medication is injected directly into the bladder muscle under local anaesthetic by the passage of a small telescope into the bladder.
The Bladder Botox at the Outpatient Clinic
The Bladder Botox at the Hornsby Outpatient Clinic offers a highly successful and comprehensive bladder program. The Clinic offers overseas all stages of the process including:
- Overactive bladder diagnosis and assessment using sophisticated urodynamic testing by an expert urologist, Dr Phillip Katelaris, to ensure accurate diagnosis
- Bladder training and pelvic floor training exercises with a specialist urological nurse, Mrs Libby King.
- Should Botox therapy be required, a walk-in walkout model has been developed for patients to undergo the procedure under local anaesthetic. Patients are able to drive home after the procedure.
Side Effects and Risks
Bladder Botox injection therapy is a very safe treatment and any side effects are mainly short-term problems that are readily resolvable.
Of course, as with any procedure, please discuss any risks with your urologist.
Mild side effects
Milder, and more common, symptoms include blood from the urine as a result of the injection, and trouble completely emptying the bladder. The blood will wear off after a few days, and in the worst-case scenario, an infection may develop, but this is easily treated with antibiotics.
The rates of urinary retention among patients are between one in 10 and one in 20. While possibly an annoyance, most patients remain largely unaffected by this, and the symptoms pass after a few weeks. In rare cases, a catheter may be required, although this too is a purely temporary measure for most.
Other potential side effects
The one major side effect that this procedure carries is extremely uncommon. In a small percentage the bladder may not empty and need to be managed. This condition does however self-correct.
If the needle enters a blood vessel in the bladder in the process of the injection, there is a very small chance that breathing may stop.
This will not occur immediately, but build up gradually and be noticed by the patient before any serious damage occurs. Once recognised, a medical professional can manage treatment to stop its progression.
Frequently Asked Questions
What are Botox Bladder Injection Treatments Like for Women?
Botox Bladder Injection Therapy can be done under local anaesthetic and a walk-in, walk out procedure for women.
Local anaesthetic cream is used in the urethra, and the bladder is injected with 100 units of Botox. This procedure takes about 10 minutes, and the patient can then walk out and drive themselves home.
About 80% will find a significant improvement in their urinary urgency and urge incontinence within two weeks, and the beneficial effect of that will last somewhere between six to twelve months, on average, about nine months
This treatment can be repeated, roughly on an annual basis.

Is an Overactive Bladder a normal part of ageing?
No. Although prevalence increases with age, Overactive Bladder Syndrome should not be considered a normal part of ageing or something that cannot be helped.
Is the prevalence of Overactive Bladder Syndrome similar in men and women?
Yes, the prevalence of Overactive Bladder Syndrome is similar in both men and women. However, Overactive Bladder Syndrome generally develops later in life in men.
Although the prevalence is similar in both gender, there are sex specific differences that exist in relation to individual OAB symptoms as well as degreee of bother and quality of life.
Should I restrict my water intake as someone with Overactive Bladder Syndrome?
No. You should continue fluid intake regularly to hold and stretch the bladder to increase its capacity.
Restricting fluid intake concentrates the urine and acts as a bladder irritant.
What is the main symptom of an Overactive Bladder?
The key defining symptom of Overactive Bladder Syndrome is:
- Urgency: The feeling of having to urgently urinate that is hard to control.
References
Arnold J, McLeod N, Thani-Gasalam R, Rashid P. Overactive bladder syndrome – management and treatment options. Aust Fam Physician. 2012 Nov;41(11):878-83. PMID: 23145420.














