
Doctor Katelaris is a highly regarded urological surgeon who performs vasectomies at the Sydney Adventist Hospital in Wahroonga and in the Urology Outpatient Clinic in Hornsby.
Table of Contents
What is a vasectomy?
A vasectomy is a simple, painless procedure and one of the safest and most effective methods of birth control. It is a safer and less expensive option than the equivalent form of contraceptive surgery for women: tubal ligation or female vasectomy, which involves an invasive operation and blocking or sealing of the fallopian tubes to prevent fertilisation.
A male vasectomy simply involves an operation that interrupts the tubes that carry sperm from the testes to the ejaculate fluid or semen (Weiske, 2001). The patient’s penis and testes are not altered, nor is there a change in hormone levels or sexual functions. Semen production, erections and ejaculations occur normally, with the only difference being that the ejaculate fluid does not contain sperm. For these reasons, approximately 10,000 men in Australia choose vasectomy every year.
Vasectomy reversal is possible; however, patients should consider the vasectomy procedure to be a permanent type of contraception when making their decision (Xiang, Luo, Cao and Yang, 2013).

Download our Vasectomy Factsheet today
Vasectomy procedure – A Gentle Approach
Assessment
The decision to undergo a male vasectomy should first and foremost be undertaken between partners in a careful, well-considered manner. It’s important that you and your partner are in agreeance on the vasectomy surgery. Relationship difficulties may arise if you feel pressured into having a vasectomy, or if you decide to have a vasectomy without agreement with your partner. Where mutual consent is lacking, a cooling-off period is recommended so you can resolve any issues and come to an agreement concerning your contraceptive practices. It is important to discuss and resolve any lingering uncertainties with a partner and doctor before undergoing the surgery.
The procedure will be discussed in person with your urologist, before your vasectomy surgery, to determine if a no-scalpel vasectomy procedure is the right option for you. Patients should be comfortable and informed about their final decision.
Before the vasectomy surgery, patients will be required to sign a consent form to ensure that they understand what is involved in the male vasectomy, including potential risks and, as with any contraceptive method, that there is no absolute guarantee for permanent sterility.
Preparing for your procedure:
For 10 days prior to your vasectomy surgery, you must not consume aspirin or other NSAIDs (non-steroidal anti-inflammatory drugs) without prior medical procedure. These medications could result in thinning of the blood and increased risk of bleeding during the procedure. Local anaesthetic will be used, so no fasting is required, and patients can drive themselves to and from the procedure.
As the procedure doesn’t require use of a general anaesthetic or sedative, no other special preparation is necessary. Patients are not advised to shave their scrotum pre-operatively as a very small area will be shaved on the operating table before the procedure.
Procedure
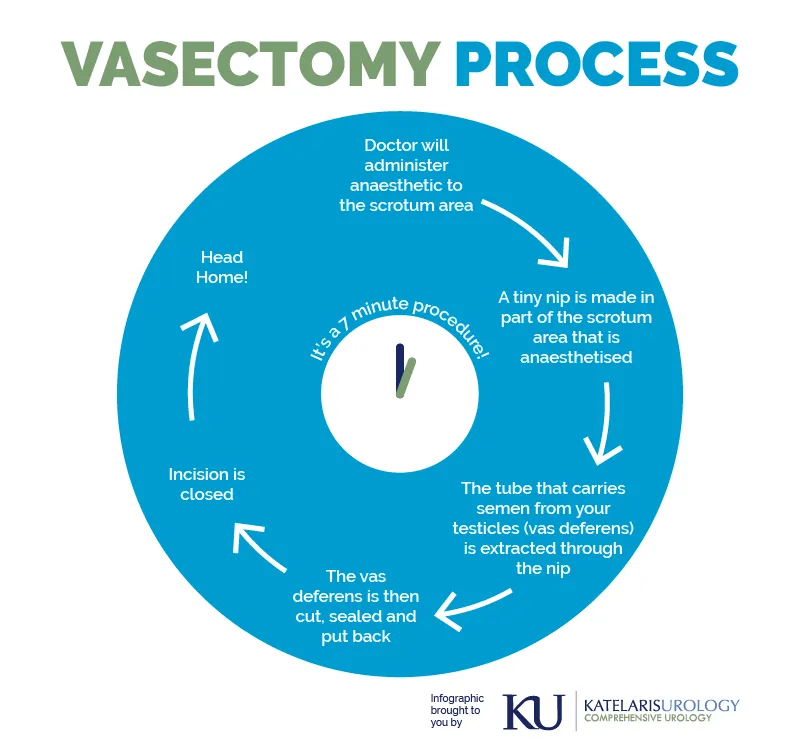
The surgical process involves a local anaesthetic and making a small incision in the skin of your scrotum. The vas deferens (tubes that carry the sperm) are located, and cut before being placed back into the body. The skin of the scrotum is then pinched and allowed to heal without the aid of stiches, leaving the incision site barely visible a few days following the procedure.
Post-operative
- Recovery
After your vasectomy surgery, you may feel sore for a few days. We recommend that you refrain from strenuous physical activity for 7 days. Sexual activity can usually be resumed a week after the procedure. - Vasectomy success rate/ResultsFollowing a vasectomy, sperm can remain in the vas deferens for weeks or even months.The first post-operative semen analysis will be performed three months after your vasectomy and following 20 ejaculations.You will not be considered sterile until two post-surgical semen tests show that no sperm remain in your vas deferens. Until your doctor has confirmed from your semen test that no sperm remains in your ejaculate, the use of other birth control must be used as a safety measure to prevent unwanted pregnancy.
Types of vasectomy
Traditional
The traditional vasectomy procedure involves blocking both the vas deferens (the tubes which carry sperm). This prevents sperm from being added to a man’s ejaculation fluid, or semen. In this procedure, a local anaesthetic is given, and one or two incisions are made in the scrotum with a scalpel. The two vas-deferens tubes are revealed, cut and sealed back up with sutures (Clenney and Higgins, 1999). The incisions in the scrotum are then closed with sutures.
Open-Ended Vasectomy
The Open-Ended vasectomy procedure was developed in 1988 to aid with epididymal congestion and testicular pressure that resulted in some patients following their operation (Errey and Edwards, 1986). This technique involves sealing the prostatic end of the cut vas deferens, but leaving the testicular end open, allowing the sperm to drain into the scrotum (Denniston and Kuehl, 1994).
No Scalpel Vasectomy (NSV)
Minimally Invasive, Effective & Reversible Birth Control
No Scalpel Vasectomy (NSV) is a safer, far less invasive vasectomy procedure, and reduces the vasectomy’s already low complication rate. Developed in China in 1974, this procedure differs from traditional vasectomy in anaesthetic administration, as well as how the two vas deferens tubes (vasa) are accessed in the body. More than 15 million men have had the procedure worldwide.
NSV uses an advanced technique to anaesthetise the scrotum more effectively than a conventional vasectomy and does not require the use of a scalpel. Instead, the physician avoids complex surgery by carefully isolating the vas deferens using the fingers of one hand (Li, Goldstein, Zhu and Huber, 1991).
In this scalpel free vasectomy, the vasa are fixed just below the scrotal skin with an instrument designed to hold firmly without pinching. A single small incision is made with pointed forceps and the vasa are delivered through the skin. After the extraction of the vasa, the tubes are cut and sealed with sutures in a conventional way. When the operation is complete, the small incision in the scrotum is simply pinched together by the physician, allowing the wound to heal itself following the procedure and negating the need for skin sutures. This scalpel free vasectomy technique also allows for a quicker recovery time (Denniston and Kuehl, 1994).
Dr Nikolas Katelaris offers no scalpel open ended vasectomy at convenient locations from the Central Coast to the CBD. Convenient clinic based vasectomy at our main office location in Hornsby. Eligible patients can use their private health insurance at day hospital locations. Click here to learn more about Dr Nikolas Katelaris.
Vasectomy Cost
Vasectomy price in Sydney depends of the vasectomy clinic and the Medicare rebate available. The out-of-pocket vasectomy cost in Sydney is approximately $900. While some GP clinics have a smaller gap – it is important to note that in these clinics the procedure is performed by a General Practitioner.
Doctor Katelaris is a specialist urologist who has performed thousands of vasectomies in Sydney and has over 35 years of experience, so you can be sure you will receive the highest quality of service.
Contact Dr. Katelaris for your no scalpel vasectomy in Sydney today.
Advantages of Vasectomy
The main advantages of a vasectomy in general include limiting the need for female birth control or the use of condoms to prevent unwanted pregnancy.
The advantages of the specialist technique used by Dr Katerlaris at Katelaris Urology, No-Scalpel Vasectomy, include the following, compared to a traditional vasectomy:
- Quick procedure (5-7 mins)
- Less discomfort
- 10 times fewer complications
- No stitches or sutures needed for healing of the skin
- Less invasive
- Shorter recovery time
Vasectomy Side Effects and Risk Factors
As with any surgical procedure, there are risk factors and side effects to consider. Your urologist will disclose these factors to you during a consultation. However, a vasectomy is generally an extremely safe and effective procedure. Very few people have complications or issues that aren’t easily treatable.

Some of the most common side effects after surgery include swelling or bleeding around the surgical site. This will typically reduce as you heal, however, if symptoms persist, you may need to revisit your urologist to have the affected areas looked at and drained.
Frequently Asked Questions
Will I be able to ejaculate after a vasectomy?
Yes, you will be able to get an erection and ejaculate like normal after a vasectomy. A vasectomy simply prevents sperm from being added to your semen. As your semen is made up of various fluids and components other than sperm, your ejaculation will not be affected, except in the fact that it should no longer cause pregnancy.
Does a vasectomy hurt?
No. You may feel some discomfort when the local anesthetic is administered, but after it takes effect, you should feel no pain. Some men may feel a slight “tugging” sensation when the vasa are manipulated and some minor discomfort may persist for a few days after surgery as your incision heals.
Post-vasectomy pain syndrome occurs in less than 1% of men. Pain following the procedure is due to either epididymal congestion or tubal obstruction. Most men find that the dull ache from post-vasectomy pain syndrome resolves with time; reassurance is all that is necessary for patients’ post-surgery. For the few men who are bothered by this discomfort in the long-term, surgical intervention may be necessary. This can include vasectomy reversal surgery, denervation of the spermatic cord or epididymectomy.
Epididymectomy is the most effective means of controlling post-vasectomy pain syndrome and involves removing the epididymis, the tubes that hold sperm in your testicles. An epididymectomy can be performed unilaterally or bilaterally, however, it will render the vasectomy irreversible on the side in question, as sperm will no longer be able to reach the reattached vas deferens.
Are vasectomies reversible?
Vasectomy reversal surgery, or vasovasostomy, is a procedure that is possible for some men to undergo. However, it is important to understand that the operation is expensive and may not guarantee a return to fertility. This is why a vasectomy must be considered a permanent procedure before the decision to proceed.
While it is possible in many cases for the cut ends of the vas deferens to be surgically reattached, it is important to ensure that the patient and their partner have decided not to have any more children before undergoing the operation.
Is there a chance of pregnancy after a vasectomy?
Yes, immediately following your procedure, it is important to continue using other forms of birth control until your urologist advises you that you are sterile. As sperm can remain in the vas deferens for weeks or even months after the vasectomy, you will not be considered sterile until two post-surgical semen tests show that no sperm remains in your vas deferens. More Details
What is the effectiveness of a vasectomy?
The efficacy of a vasectomy as a method of contraception, in preventing pregnancy, is 99%, however, it usually takes around 3 months following the procedure for all of the sperm to clear from your ejaculate. Until your specialist confirms that you are sterile with a semen test, it is recommended to continue using other forms of contraception. This is because there may still be some sperm cells in the upper part of the tubes and it can take several months for them to flush out. Contraception can only be discontinued once a test shows that the semen has a zero sperm count.
In rare cases sperm may still manage to travel across where the tubes have been cut. No vasectomy can be guaranteed 100% as a contraceptive. The chances of pregnancy following the procedure are around 1 in 1,000.
Sperm may continue to be made in the testes after vasectomy, but after a length of time production may be reduced or may cease. Once the production of sperm has ended, a reversal procedure will not be feasible.
How long does a vasectomy take?
A No-Scalpel Vasectomy (NSV) performed by Dr Katelaris will take between 5-7 minutes.
Once you are comfortable, a local anesthetic will be administered. Following this, Dr Katelaris will make a small incision in the skin of your scrotum, locate your vas deferens and cut them, before stitching the two ends of the tubes back up and returning them to your scrotum. The incision in your scrotum does not require stitches in this method and will simply heal by itself in the days following your procedure. As no sedative is involved in this surgery, you can drive yourself home after the procedure with minimal discomfort.
Is a vasectomy permanent?
A vasectomy should be considered a permanent form of contraception between a patient and their partner. Although many vasectomies can be reversed, this procedure is expensive and may not guarantee restored fertility.
How much does a vasectomy cost?
A vasectomy is a Medicare rebated procedure, with the out-of-pocket cost approximately $900. Some GP clinics have a smaller gap – however, it’s important to note that in these clinics the procedure is performed by a General Practitioner. Doctor Katelaris is a specialist urologist who has performed thousands of vasectomies and has over 35 years of experience, so you can be sure you will receive the highest quality of service.
Will vasectomy affect my libido?
No! A vasectomy does not alter your hormones in any way, so there will be no change in your sexual function or libido. The only change you will be required to implement in your sexual activity is waiting 1-2 weeks post-surgery for your surgery site to heal. More Details
How long after a vasectomy can you have sex?
Normal sexual activity can usually be resumed after 1-2 weeks post-surgery once the incision has had time to heal. Patients must consider, however, that they may not be deemed sterile for weeks or even months after their procedure, so it is important to continue using other forms of contraception until sterility is confirmed by your specialist.
Signs your vasectomy has grown back together?
Recanalization is a rare occurrence where the vas deferens find an alternate route to reconnect with each other and the sperm are able to enter the ejaculate fluid again. This can be determined by your urologist using a semen test, and is important to ensure a vasectomy has been successful and resulted in sterility.
How does vasectomy prevent pregnancy?
A vasectomy prevents pregnancy by preventing sperm from being added to your semen or ejaculate. Your semen is made up of various different fluids, nutrients and other components, including sperm. Sperm is carried from the site of production in the testes to the semen via two tubes called the vas deferens. A vasectomy cuts and seals the vas deferens, preventing the sperm from being added to the semen and leaving the penis in the form of ejaculate. Unreleased sperm is naturally absorbed by the body as is would in normal circumstances.
Do you produce less sperm after vasectomy?
There is a chance for men to produce less sperm over time after a vasectomy. This is why vasectomy reversal surgery is recommended within 10 years of the operation, to increase the chances of a normal return to fertility. For this reason, it is also important for a man and their partner to confirm their understanding that a vasectomy is a permanent form of birth control and their fertility may not fully return if the procedure is later reversed.
How safe is a vasectomy?
A vasectomy is an incredibly safe and effective procedure, however, as with any surgery, it can come with risks and side effects which your urologist will confirm with you during a consultation. Very few people have complications or issues that aren’t easily treatable. Some of the more common side effects after surgery include swelling or bleeding around the surgical site. This will reduce as your wound heals, however, if it doesn’t you may need to revisit your urologist who will drain the affected area of fluid to reduce the swelling.
What are the side effects of a vasectomy?
As with any surgical procedure or method of contraception, a vasectomy carries some risks alongside its benefits. While a vasectomy is a very low risk procedure, some complications are possible in rare situations. The most common side effects of vasectomy surgery are listed below:
- Hematoma (bleeding) and infections are the most common complications of vasectomy, although the risk of this is a lot less, approximately 1%, when using the No-Scalpel Vasectomy technique. As this method only requires a small incision site, there is minimal effect on the blood vessels in the scrotum, which are usually responsible for post-surgical bleeding.
- Recanalization, or vasectomy failure, is another possible risk to consider when undergoing the procedure. Even when performed without complications, a vasectomy is not guaranteed to be 100% effective. It is possible in rare cases for sperm to find an alternate way to cross the space between the two blocked ends of the vas deferens. Recanalization is why it is important to collect semen samples 6-8 weeks post-vasectomy to confirm that no sperm is present in the semen. Recanalization usually occurs in the first 2-3 months after vasectomy, however, in very rare cases, it can occur years later.
- Sperm granuloma, a hard, sometimes painful lump about the size of a pea, may occur as a result of sperm leaking from the cut vas deferens. This lump is not dangerous and is absorbed by the body over time.
- Congestion caused by sperm in the tested and epididymis may result in a sense of pressure or discomfort for 2-12 weeks after a vasectomy. This condition will also resolve itself over time, however, if symptoms persist, please consult your urologist.
What are the advantages of a vasectomy?
The main advantage of a vasectomy is to prevent pregnancy without the need for various forms of birth control, such as condoms, female hormonal contraception or female invasive surgery.
References:
Clenney, T.L. and Higgins, J.C., 1999. Vasectomy techniques. American Family Physician, 60(1), p.137.
Denniston, G.C. and Kuehl, L., 1994. Open-ended vasectomy: approaching the ideal technique. The Journal of the American Board of Family Practice, 7(4), pp.285-287.
Errey, B.B. and Edwards, I.S., 1986. Open-ended vasectomy: an assessment. Fertility and sterility, 45(6), pp.843-846.
Li, S., Goldstein, M., Zhu, J. and Huber, D., 1991. The no-scalpel vasectomy. The Journal of urology, 145(2), pp.341-344.
Weiske, W.H., 2001. Vasectomy. Andrologia, 33(3), pp.125-134.
Xiang, Y., Luo, P., Cao, Y. and Yang, Z.W., 2013. Long-term effect of vasectomy on spermatogenesis in men: a morphometric study. Asian journal of andrology, 15(3), p.434.
















