In Australia, 15% of men and up to 37% of women experience some form of incontinence. It can be an embarrassing problem and many people delay getting the help they need and don’t realise that there are many solutions available. Most people that suffer from incontinence can be successfully treated.
What is Urinary Incontinence?
Urinary incontinence is the involuntary loss of urine from the body. When the muscle (sphincter) that holds the bladder neck closed is not strong enough to retain urine in the bladder, the result is urinary incontinence.
Incontinence may occur when:
- The muscle is too weak.
- The bladder muscles contract too strongly and at the wrong time.
- The bladder is not emptied regularly or completely.
What Causes Urinary Incontinence?
The main urinary incontinence causes are:
- Trauma to the pelvis, e.g., childbirth or prostate removal surgery.
- Infections.
- Medications, such as sleeping pills.
- Spinal cord injury or nerve damage.
- Ageing.
- Overactive bladder activity.
- Neurological disorders that interrupt the normal signals between the bladder and the brain including illnesses such as multiple sclerosis or Parkinson’s disease.
What Are the Types of Urinary Incontinence?
There are three main types of urinary incontinence.
 |
Urge IncontinenceWhen the bladder contracts at the wrong time giving you the feeling that you have to urinate immediately even if you have just emptied your bladder. |
 |
Overflow IncontinenceCaused by the leakage of urine from an overly full bladder and it occurs in patients where the bladder outflow is obstructed or the detrusor muscle is simply too weak to allow the bladder to empty properly. There is often no sensation of needing to void. |
 |
Stress IncontinenceThe accidental release of urine when pressure is applied to the bladder, such as when you cough, sneeze, laugh or lift something heavy. It is caused by weakness of the sphincter muscle. |
There are two other minor types of Urinary Incontinence are:
- Mixed Incontinence: Mixed Incontinence is usually considered a combination of stress incontinence and urgency incontinence.
- Functional Incontinence: Known also as disability associated urinary incontinence. This occurs when an individual’s bladder is working normally but are unable to access the toilet due to a cognitive or physical condition.
Diagnosing Urinary Incontinence
Incontinence is diagnosed with some or all of the following tests:
Urinalysis and Urine Culture |
Urodynamic Study |
Cystoscopy |
|
Your GP may have performed this test already. This test is to check whether your incontinence is the result of an infection in the urinary tract or whether you have other symptoms like microscopic haematuria. |
These tests are performed in our outpatient clinic, and involve:
|
Sometimes diagnosis will involve inserting a scope to examine your bladder’s health and condition. These procedures can be performed in the Urology Outpatient Clinic. |
Katelaris Urology: Effectively Managing Incontinence
The key to modern incontinence management is accurate diagnosis. Particularly common in women, a mix of urinary incontinence is under-reported and under-treated due to the lack of complex tools, such as a urodynamic assessment.
At Katelarius Urology, sophisticated computerised urodynamic equipment is used to make an accurate diagnosis which is then used to effectively guide and provide correct information on management.
The majority of people with bladder control problems can improve their condition. Even those who are suffering from urinary incontinence post prostatectomy can look forward to being better.
Many different stress incontinence treatments are readily available including:
- Pelvic floor training
- Male and Female sub urethral sling surgery
- Implantation of an artificial urinary sphincter
- Botox Therapy
- Neuromuscular stimulation
- Urinary Incontinence Medication
- Pharmaceutical Agents
Male Urinary Incontinence
Urine leakage in men is common, but it is often related to prostate problems. As men age, the prostate gland grows larger, squeezing the urethra and pushing the neck of the bladder out of position.
On many occasions, male urinary incontinence negatively affects quality of life and is associated with a serious psychosexual and social burden. However, there are readily available male urinary incontinence treatments that are minimally invasive surgeries.
There are two main types of urinary incontinence treatment for elderly males and adult males.
- The Sling Procedure
- Artificial Urinary Sphincter
The Sling Procedure
| Male Sling surgery is the most common procedure as male urinary incontinence treatment. It is suitable for men with mild to moderate stress incontinence that has not responded to conservative measures. |
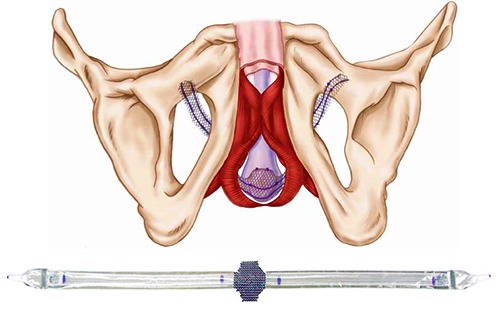 The male sling involves insertion of a mesh sling beneath the urethra for added support. |
| Surgery Duration | This procedure is usually performed as a short-day procedure at the Sydney Adventist Hospital but occasionally an overnight stay may be necessary. |
| How the Sling Procedure works |
Some slings work slightly differently where their placement results in increased pressure on the urethra to decrease the possibility of urine leakage. |
| Post-Procedure |
|
You should contact Doctor Katelaris immediately should any problems occur after surgery, especially if you are experiencing:
- High Temperature
- Inflammation
- Excessive Pain
- Redness in the Surgical Area
Artificial Urinary Sphincter
| The Artificial Urinary Sphincter is the highest standard of treatment for male urinary incontinence. It is particularly effective for more severe types of male urinary incontinence, where circumferential compression of the urethra is required. |
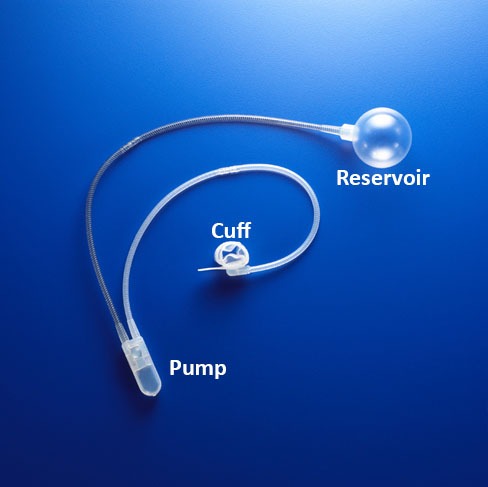 The Artificial Urinary Sphincter is constructed of biocompatible silicon and consists of three main components, a reservoir, a cuff and a pump. |
| Surgery Duration | This procedure is a short procedure, but you can expect to be discharged after a short, 24 hour stay in the Sydney Adventist Hospital. |
| How the Artificial Urinary Sphincter works |
|
| Post-Procedure |
|
You should contact Doctor Katelaris immediately should any problems occur after surgery, especially if you are experiencing:
- High Temperature
- Fever
- Unusual or prolonged pain, redness, swelling or rash near the incision or scrotum
- Pus coming from the surgical incision
- Problems with urination
- Any part of the device is visible through the skin
- Inability to locate the control pump
Female Urinary Incontinence
Urinary incontinence in women is very common, often a consequence of childbirth or ageing. It can be a significant cause of embarrassment and loss of quality of life. However female urinary incontinence is a readily treatable condition, and for many women cure is possible.
There are non-surgical and surgical options for treatment for urinary incontinence in elderly females and adult females. These two options are:
- Non-Surgical Treatment: Pelvic Floor Training
- Surgical Treatment: Sub Urethral Sling Surgery
Pelvic Floor Training
| Pelvic Floor Training is often the first means of managing stress urinary incontinence caused by weakness of the pelvic floor. |
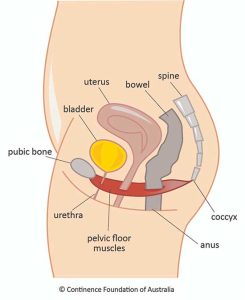 A woman’s pelvic floor muscles support the bladder, bowel, and uterus. The urethra, anus and vagina all pass through the pelvic floor muscles. |
| What Pelvic Floor Training is |
The pelvic floor muscles are a group of muscles that attach to the lower bones of the pelvis. The outlet from the bladder, called the urethra, passes through the pelvic floor and so contraction of these muscles can assist in compensating for incontinence. When the pelvic floor is contracted the muscles increase support of the pelvic organs and tighten the urinary sphincter. |
| Where you can access Pelvic Floor Training |
Pelvic floor and bladder training is available at the Urological Outpatients Clinic under the supervision of our continence nurse. She will assist you in correctly identifying your pelvic floor and teach you the correct technique for performing strengthening exercises. |
Sub Urethral Sling Surgery
| Surgery for female urinary incontinence is usually in the form of sub urethral sling surgery – a very major advance in the management of female incontinence and for appropriately selected women, can offer cure rates of 80 to 85% |
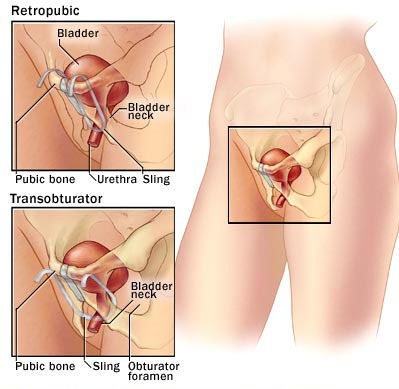 Suburethral slings all work to improve support to the urethra, similar to the normal function of the pelvic floor, which helps to prevent urine leakage during activities and straining. |
| Surgery Duration | The surgery is minimally invasive and involves a short 24 hour stay in hospital. |
| What Sub Urethral Sling Surgery is |
There are a variety of slings available and the best choice for you will be discussed at a pre-operative consultation. However, a traditional sub urethral sling operation requires a combined abdominal and vaginal approach, and can be made from with biological or synthetic materials. Strips of material are tunnelled under the urethra and are attached to the rectus muscle or to the iliopectineal ligaments. |
| Where you can access a Sub Urethral Sling Surgery |
You can contact our friendly staff to get a quotation for a sub urethral sling procedure and book a surgery here. |
| Post-Procedure |
|
You should contact Doctor Katelaris immediately should any problems occur after surgery, especially if you are experiencing:
- High Temperature
- Inflammation
- Excessive Pain
- Redness in the Surgical Area
Katelaris Urology: Managing Incontinence
Urinary incontinence is not only a significant health problem in Australia, it is also a significant problem worldwide.3 At Katelaris Urology, we are ready to assist our patients with their concerns and support them with a multitude of treatments based on their condition.
As technology paves the way for sophisticated urinary incontinence assessment and accurate diagnosis, our patients have access to faster, more conclusive results than in the previous years. On top of this, patients now have a wide range of incontinence solutions that fit their budget and preference.
With these resources available, both men and women should feel confident to mention the problem to their doctors in order to avail of modern diagnostic techniques and treatments.
If you have any issues you’d like to get resolved and you’re looking for an incontinence treatment in Australia, you can contact our friendly staff for a second opinion here.
Frequently Asked Questions
Can Urine Incontinence Be Cured?
Yes, all types of Urine Incontinence can be cured or treated. However, your treatment will depend on the severity of your case.
There are three main treatments are:
- Conservation Therapy
- Oral Medication
- Bladder Botox Injection
What Are the First Signs of Incontinence?
The first signs you should look for are:
- Problems passing urine.
- A slow stream of urine.
- Straining or passing urine.
- Stopping and starting as you pass urine.
- Problems after you have passed urine, e.g., the feeling that you have not completely emptied your bladder after you think you have finished.
If you are experiencing these symptoms, don’t hesitate to contact us for an enquiry or a second opinion.
How Do I Know if My Urinary Incontinence is Serious?
It’s important to reach out to a doctor if your Urinary Incontinence is regular or is affecting your quality of life.
Leaving it untreated can result in you restricting your activities and limiting your social interactions, which will drastically lower your quality of life.
If you believe your Urinary Incontinence has become serious, contact us to get in touch today and receive a professional opinion.
How Can You Fix Urinary Incontinence?
Urinary Incontinence can potentially be resolved through these treatments, depending on the severity.
The four main Overactive Bladder treatments include:
- Bladder Retraining
- Pelvic Floor Training
- Urinary Incontinence Medication
- Bladder Botox Therapy
To learn more about the treatments available to fix Urinary Incontinence, visit our Overactive Bladder page.
What is The Most Effective Treatment for Incontinence?
In many cases, the most effective treatment depends on the severity of your Urinary Incontinence.
However, when it comes to severe cases of Urinary Incontinence, Bladder Botox Therapy has been seen to be the most effective remedy with the results showing that:
- The majority of patients had at least a 50% reduction of daily leakage episodes
- Around half reduced their leakage episodes by 75%
- 1 in 4 patients reported no leakage at 12 weeks
- All studies reported significant responses to Botox when compared
What Causes Urinary Urgency in Men?
There are a number of factors that male incontinence can be caused by.
These include:
- Prostatitis: A painful inflammation of the prostate gland
- Injury or damage to nerves or muscles from a previous surgery
- An enlarged prostate gland, which can lead to benign prostate hyperplasia.
Urinary Incontinence surgery for males is readily available and accessible. If you are interested in getting a quote or understanding what surgery would suit your situation, you can contact us here.
What causes a female to pee a lot?
References
- Hawthorne G. Measuring Incontinence in Australia. Commonwealth of Australia; 2006.
- Porena, M., Costantini, E. & Lazzeri, M. Mixed Incontinence: How Best to Manage It?. Curr Bladder Dysfunct Rep 8, 7–12 (2013). https://doi.org/10.1007/s11884-012-0161-8
- Nitti VW. The prevalence of urinary incontinence. Rev Urol. 2001;3 Suppl 1(Suppl 1):S2-6. PMID: 16985992; PMCID: PMC1476070.


