Make sure this is the right option for you and your partner:
A vasectomy is a safe and effective form of permanent birth control that over 10,000 men in Australia choose to undergo every year. The routine procedure involves severing the vas deferens tubes to prevent sperm from travelling to the testes and penis.
If you are considering having a male vasectomy, there are a few important aspects to consider before proceeding. Firstly, it is important to discuss with your partner the reasons behind your decision, one of which may be birth control. When considering a vasectomy, it is important to be sure that you do not want to father children in the future, as a successful vasectomy reversal cannot be guaranteed. If you have any doubts about wanting children, it may be worth investigating another less permanent form of contraception that would be more appropriate.
It is important to always be informed of the facts surrounding a medical procedure, even a simple and safe surgery such as a vasectomy. Read on for some vasectomy procedure facts that might surprise you…
A vasectomy is a short and quick procedure:
A vasectomy should take no longer than 20 minutes, including preparation and discharge.
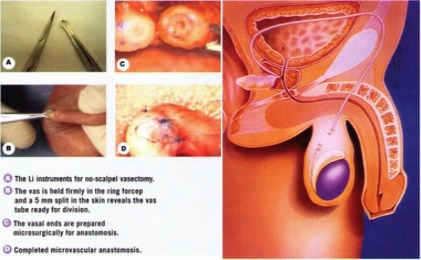
A conventional male vasectomy involves shaving a small area of the scrotum, administering a local anaesthetic and making incisions in the scrotum, followed by locating and cutting the tubes and closing with stitches.
A more modern procedure is that of a no-scalpel vasectomy, which is safer and minimally invasive. It involves more effective anaesthesia and making tiny incisions with pointed forceps in the scrotum which require no stitching afterwards. This method takes only a few minutes and has a much lower complication rate than for a conventional vasectomy.
The surgery itself takes 5-7 minutes, during which the doctor will:
-
- Make a small incision in the skin of the scrotum
- Extract the vas deferens (the tubes that carry sperm) and severe them
- Seal the vas deferens and put them back in the scrotum
- Close the scrotum incision
That’s it, nothing more to it.
This “no scalpel, no stitches” method has been proven to reduce bleeding and lower the risk of infection, bruising, and other complications. Because local anaesthetic is used, you can drive yourself right home afterwards, although you will need to rest for a couple of days.
Where to have it done
Vasectomies can be done at a public hospital by a GP, however, there is usually a waiting list involved. Should you choose to have your vasectomy performed privately at a urology clinic, you vasectomy will be conducted by an experienced microsurgeon, leading to fewer complications and a higher success rate should you undergo a vasectomy reversal. A vasectomy performed at a clinic usually only requires a day stay, and if you opt for a no-scalpel vasectomy, it can be done within minutes. When preparing for your vasectomy, there are no fasting requirements prior to your procedure, and most men should be able to drive themselves home afterwards.
If you would like to find out more about a male vasectomy, consult with a qualified urologist to discuss the procedure and whether it is right for your circumstances.
A vasectomy is generally a safe, painless and effective procedure:
Any surgical procedure can feel a little daunting, especially one that involves the genital region, however, there is nothing to fear from having a vasectomy. For patient comfort, the procedure is conducted by a urologist under local anaesthetic – meaning the scrotum area will be numbed directly, while the remainder of your body is unaffected. This means that when the procedure is performed, you will not feel anything. If needed, you can also opt to receive some medications to reduce anxiety while the vasectomy takes place.
The recovery time post-vasectomy is very fast with minimal side effects:
If you’ve just searched “what should I expect after a vasectomy?” or “vasectomy recovery” on Google, then you have landed on the right page. Here’s what to do after a vasectomy surgery if you want to recover quickly.
How Long Does It Take to Recover from a Vasectomy Fully?
Generally, there is very little pain or discomfort following a vasectomy. You can usually make a return to work within 2-3 days, and resume normal exercise routines within 7 days. Sexual activity can aslo be resumed after a week, however, it is important to use some form of contraception, as it can take months after a vasectomy to become sterile.
What to Do After a Vasectomy Surgery?
- Keep Yourself Clean
It can be possible to catch an infection after a male vasectomy surgery if you don’t keep the surgical site clean. You can shower 24 hours after your surgery, but make sure to clean yourself with a wet towel before then as it is normal for sweat to build up in that area. Change your clothes every day and make sure that your underwear isn’t too tight as this may cause additional discomfort and increase the build-up of sweat. You must also avoid exercise for 7 days as this will increase sweating and may cause blood to seep into your scrotum.
- Get Lots of Rest
One of the best ways to recover from this surgery is to get as much rest as you can. It will help you recover faster, and it will prevent the incisions from reopening. Try to lie down on your back as much as possible instead of sitting upright. Lying down will reduce the strain on your scrotum. You should even consider raising your feet a bit so that your blood circulation is better and applying ice packs to the affected area.
Long Term Effects and Complications
One of the most common questions regarding a vasectomy is about side effects or long term complications. While the risks involved in vasectomies are very low, they should still be taken into consideration.
Apart from mild pain and discomfort during recovery, very few men who undergo a vasectomy experience noticeable side effects. Some abdominal pain after a vasectomy may be present, however, it usually subsides quickly. Other surgery related side effects can include swelling, bruising or infection at the site, which will usually disappear within two weeks.
Some men report gaining some weight in the months following a vasectomy, but generally, their weight returns to its normal state after a while. The weight gain could be due to limiting exercise after the procedure to rest and recover, however, there is no reason not to return to a normal and active routine a week after having a vasectomy.
Having a vasectomy will not affect your sexual functioning, performance or enjoyment:
A successful vasectomy should not interfere with a patient’s enjoyment of sex with a partner. You can start having sex a week after your surgery, however, you must make sure to use some form of contraception. This is because there will still be some sperm in your semen when you ejaculate. It could take up to several months to become completely sterile.
After a vasectomy, sex will be just as pleasurable as it’s ever been and your sexual performance will not be hampered by the procedure. Additionally, an ejaculation will still look and feel the same, with the only difference being the absence of sperm.
Sterilisation doesn’t happen immediately after a vasectomy:
Keep in mind that complete sterilisation doesn’t happen immediately following a vasectomy procedure. Some sperm can remain present in the tubes for up to three months. This means that other types of contraception should be used until tests show the all-clear. Your sperm count will experience a gradual decrease, and it can take several months to become sperm-free. During that time, continue to practice other birth control methods to avoid an unplanned pregnancy.
A vasectomy can be reversed, but should be considered a permanent form of contraceptive
Vasectomy reversal surgery is a procedure that can be successful in the majority of patients. It involves the reconnection of the vas deferens by a micro surgeon. The success rate of reversal depends on several factors including the type of vasectomy, how long it’s been since the vasectomy took place, but a very high percentage of men do successfully become fertile again.
Katelaris Urology is here to answer any questions or concerns you may have about the vasectomy procedure, so put your mind at ease by getting in touch today for a consultation.